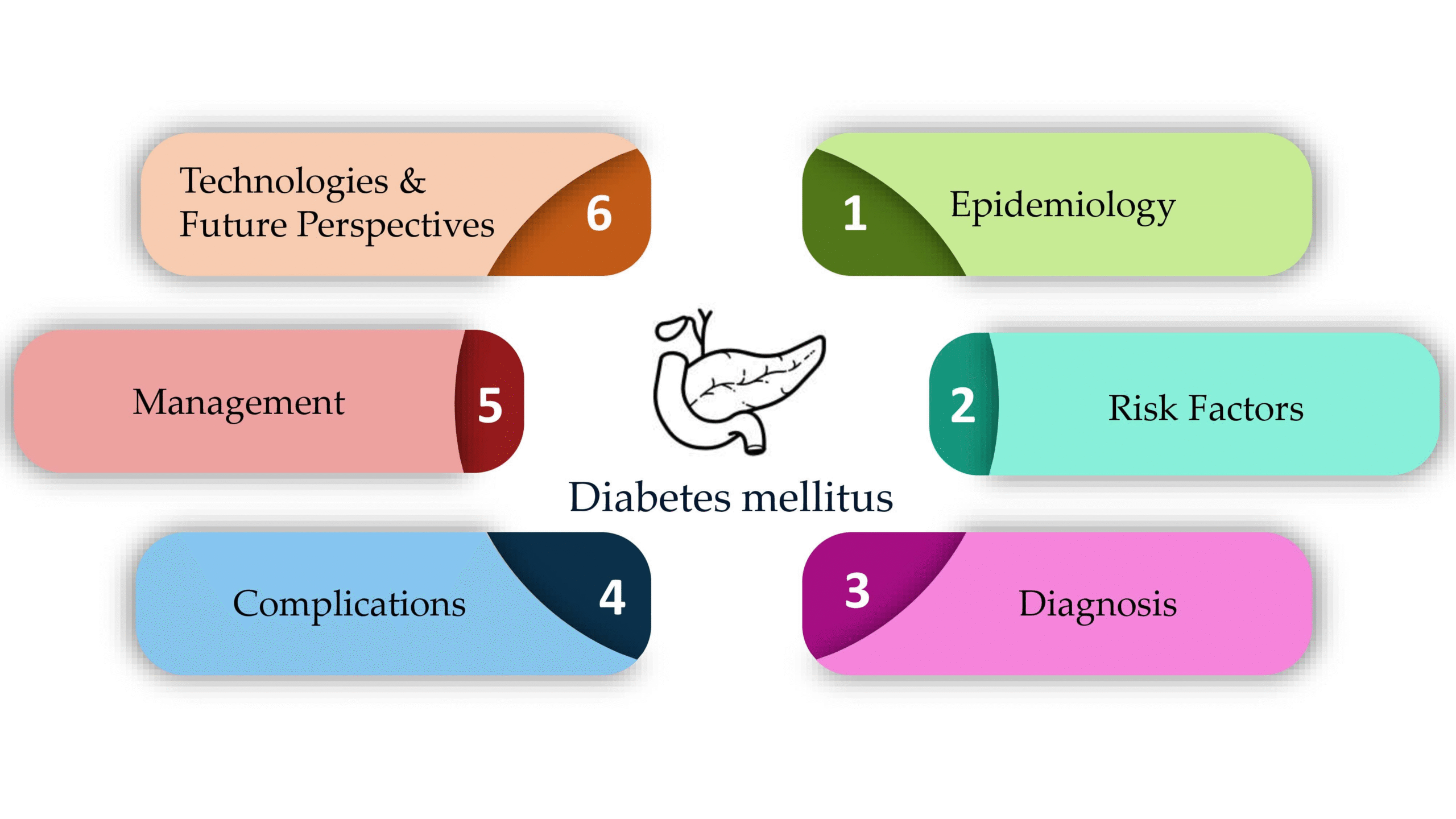
What is Diabetes Mellitus?
Diabetes Mellitus is a condition where the pancreas produces insufficient or no insulin, a hormone essential for helping the body’s cells absorb glucose (sugar) to use as energy. It can also occur when the body’s muscle, fat, and liver cells don’t respond properly to insulin. As a result, glucose builds up in the bloodstream and urine, leading to symptoms like excessive thirst, hunger, urination, and issues with fat and protein metabolism.
Diabetes Mellitus differs from diabetes insipidus, which is caused by a lack of the hormone vasopressin, affecting the regulation of urine production.
Risk Factors and Demographics
Diabetes is more common among people over the age of 45, those who are overweight or physically inactive, and individuals with a family history of diabetes. It is also more prevalent in people of African, Hispanic, and Native American descent, with Native Americans having the highest diabetes rate worldwide. Women are more likely to be diagnosed with diabetes than men.

Types of Diabetes
-
Type 1 Diabetes: This form of diabetes typically starts in childhood and results from the pancreas stopping insulin production altogether. It’s also known as insulin-dependent diabetes.
-
Type 2 Diabetes: Usually occurring in adulthood (though it can appear in teenagers), the pancreas still produces some insulin, but either it’s insufficient or the body doesn’t use it effectively. This form is also called non-insulin-dependent diabetes.
Diagnosing Diabetes
Diabetes is often diagnosed by measuring blood glucose levels after fasting for about eight hours. In some cases, doctors use an oral glucose tolerance test, which measures glucose levels before and after consuming a certain amount of sugar. There’s also a promising test being developed for Type 1 diabetes, which identifies antibodies specific to the disease, potentially allowing for early detection.
Treatment and Management
Once diagnosed, diabetes is managed by regulating blood glucose levels and preventing complications. Treatment varies by diabetes type and may include insulin therapy, medication, lifestyle changes, diet, and regular exercise.
-
Type 1 Diabetes: Patients need insulin injections (2-4 times per day), as their body does not produce insulin. The insulin dosage varies by individual, influenced by physical activity, diet, and any other health conditions. People with Type 1 diabetes regularly monitor their glucose levels using a blood glucose meter and adjust insulin, exercise, and food intake accordingly. Meal timing and the type of foods consumed are also crucial in managing the condition.
-
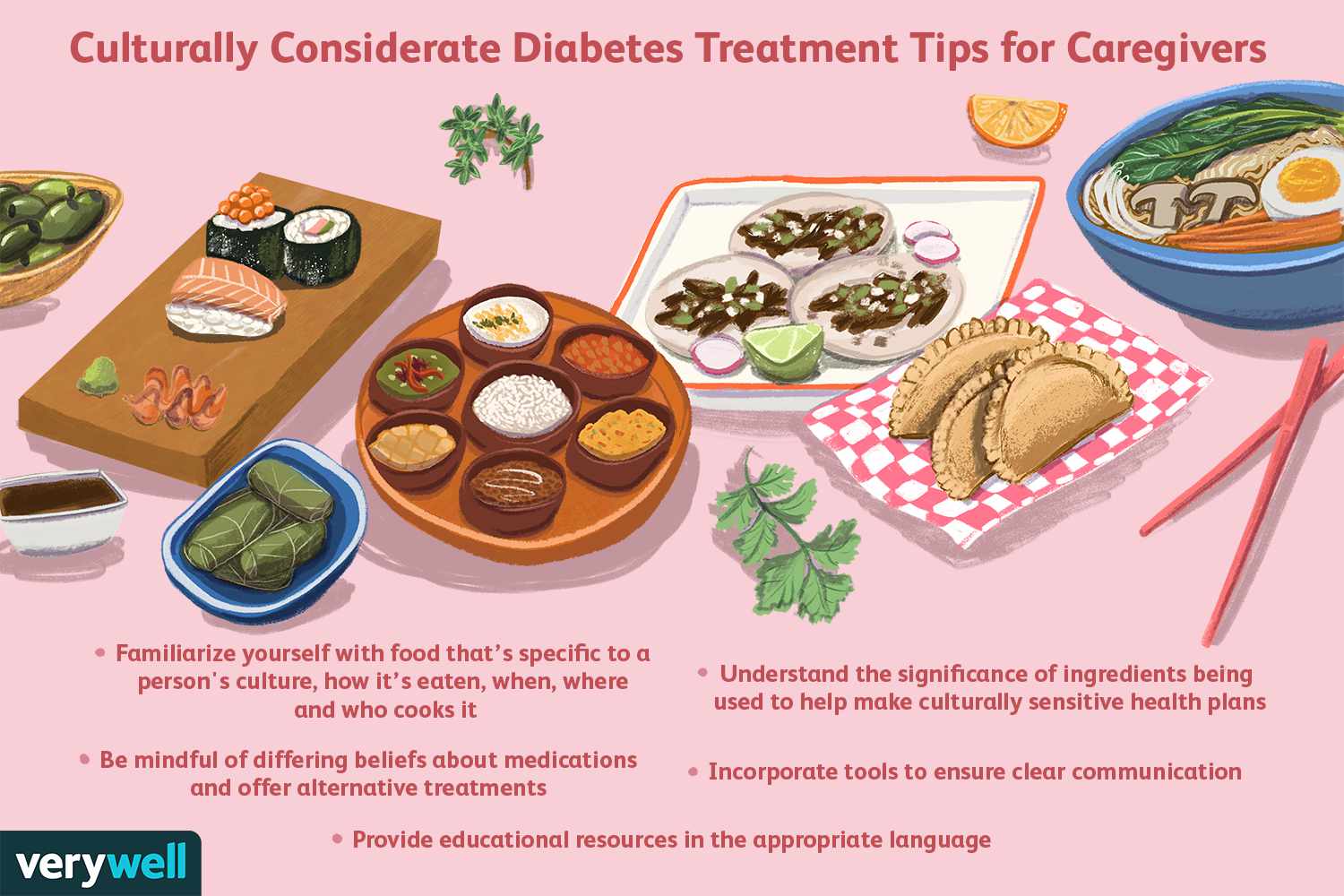
Type 2 Diabetes: The initial treatment for Type 2 involves diet control, exercise, and weight management. In some cases, medication may be required if these steps are not enough. A typical diet plan emphasizes foods low in fat (under 30% of total calories), moderate protein (10-20% of total calories), and includes a variety of carbohydrates like beans, vegetables, and grains. Exercise, even small amounts, helps cells absorb glucose and can improve insulin sensitivity. Regular weight loss can also partially reverse the body’s difficulty in using insulin.
Both types of diabetes require close monitoring of blood sugar levels and a carefully balanced approach to lifestyle and dietary habits.